What are the risks and complications associated with this surgery?
As with any other major surgery, there are some potential risks after knee replacement surgery. Overall the incidence of complications after knee replacement surgery is fortunately quite low. The possible complications are:
1) Deep venous thrombosis (DVT)
DVT is common after any major surgery on the lower limbs or pelvis including joint replacement surgery. Though DVT is quite common after joint replacement surgery it does not cause any symptoms in majority of the patients. In a small proportion of patients (less than 1%) the clot can dislodge and cause blockage of major blood vessels in the lungs (pulmonary embolism) or in the brain (cerebral embolism). In such an eventuality patients need supportive therapy in the intensive care (ICU). After total knee replacement surgery, patients are usually put on low molecular weight heparin (LMWH) injections which function as blood thinners and reduce the incidence of DVT and its consequences. Additionally patients are also given elastic stockings (TED stockings) in the post-operative period. After the surgery, all efforts are made to minimize the risk of DVT. The followings methods are commonly employed:
1. Low molecular weight heparin (LMWH) – Blood thinning injections
2. Warfarin or Aspirin – Blood thinning tablets
3. Elastic stocking – TED stockings
4. Intermittent pneumatic compression pumps – Flowtron pump
5. Early mobilization – getting a patient out of bed as soon as possible
Usually a combination of methods is used to prevent clot formation.
2) Infection
As with any other major surgery, there is a potential risk of infection with any joint replacement surgery. The overall risk of infection with modern techniques is quite low (about 1-2 %). Every effort is made to prevent infection after a joint replacement surgery.
How does one reduce the chances of infection after joint replacement surgery?
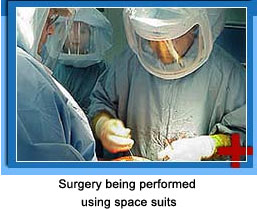
Every patient is assessed carefully before surgery for risk of infection. Patients with pre-existing diabetes have a higher chance of infection and need good control of their blood sugar levels. Patients with urinary tract infection, bad teeth or with any other infection in the body should wait until their infection is treated and cleared. Patients are given higher antibiotics during and immediately after surgery as a precautionary measure (prophylactic antibiotics). These surgeries are performed in clean air operating theatres with laminar airflow and body exhaust suits.
What happens if a patient develops infection after joint replacement?
The treatment of infection after joint replacement depends on whether the infection is superficial or deep. Most superficial infections can be treated with a prolonged course of antibiotics (6-8 weeks) given intravenously initially and later orally. Deep infections which present early (within 3-6 weeks after surgery) need immediate arthrotomy and wash out (opening of the wound and washing out of the wound with normal saline) followed by prolonged antibiotic therapy. When treated early it is possible to retain the patients’ prosthesis and expect control of infection. It is therefore very important to act swiftly once there is any suspicion of an infection. Deep infections which present late may need two stage surgeries whereby the existing prosthesis is removed in first stage followed by antibiotics for about 6-8 weeks to control infection. Once the infection is under control, a new prosthesis can be implanted during the second stage of surgery. In some instances where the infection is difficult to control, it may be necessary to consider arthrodesis of the joint (joint fusion).
3) Stiffness
Though most patients are able to bend their knees to beyond 100 degrees after a good rehabilitation program, some patients tend to have stiff knees despite proper rehabilitation. It should be emphasized that the range of movement (ROM) that a patient can expect after a knee replacement depends on the pre-operative range of movement in the knee. Most patients can expect to get 10-20 degrees more movement as compared to the pre-operative range. Some patients have a tendency to develop excessive scarring in the knee after surgery (arthrofibrosis) and these patients may have severe stiffness in the post-operative period. These patients should be considered for manipulation under an anaesthetic (MUA) to break down the adhesions followed by vigorous physiotherapy.
4) Loosening, Implant wear and Osteolysis
Loosening of the prosthesis is due to the bond between the implant-cement-bone becoming weak. This is long term complication which can be seen with any joint replacement surgery over a period of time. Patients who are overweight, those who have had an infection in the post-operative period, patients with severe osteoporosis, patients who have residual instability or a deformity in the knee (like varus deformity) after surgery, and young and active patients who tend to load their joints excessively tend to develop implant loosening earlier.
Implant wear relates to wearing out of the polyethylene (plastic liner) between the femur and tibia. This again is long term complication with any joint replacement surgery especially where polyethylene is used. Patients who have persistent deformity after surgery (varus deformity) or those with some residual instability after surgery tend to have accelerated poly wear. This leads to release of microscopic debris being released in the joint which in turn stimulates the release of certain bio-chemicals in the joint which can cause osteolysis (eating away of bone around the prosthesis). This can lead to early loosening of implants or peri-prosthetic fractures (fractures around the implant).
Patients who progressive loosening, and those with excessive wear will require revision knee replacement surgery. Those with a peri-prosthetic fracture will need internal fixation or revision knee replacement using long stem prosthesis.