What is Frozen shoulder?
Frozen shoulder is a condition in which the shoulder becomes markedly painful and stiff (loses its movement). It may follow an injury to the shoulder, but may also arise gradually without any injury. It also known as periarthritis or adhesive capsulitis.
What causes Frozen Shoulder?
The exact cause of this condition is still not very well understood. There is It is associated with severe inflammation of the shoulder joint capsule (causing pain) which leads to adhesions in and around the joint and contracture of the capsule (causing restriction of movements). This may occur spontaneously or following a trivial injury to the shoulder. It may be also be secondary to tendinitis (inflammation of a tendon) or, bursitis (inflammation of a bursa) or rotator cuff tear. It may follow after surgery on the shoulder or after prolonged shoulder immobilization. Patients with diabetes, stroke, lung disease, rheumatoid arthritis and hyperthyroidism are at a higher risk of developing frozen shoulder. In some patients frozen shoulder is associated with a pain syndrome called ‘reflex sympathetic dystrophy’ (RSD).
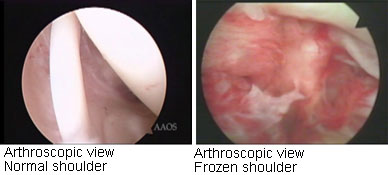
How do you diagnose frozen shoulder?
The diagnosis of frozen shoulder is made on the basis of patient’s symptoms and physical examination.
Frozen shoulder usually occurs between the age of 40 and 65 years and is more common in women than men. It usually affects the non-dominant arm (i.e. the left arm in a right-handed patient and vice versa), and in 10-15% of patients it may affect both shoulders at the same time. Patients will have severe pain and stiffness (restriction of all movements in the shoulder). The pain is typically present at rest and even at night. Physical examination of a frozen shoulder reveals limitation of both active (patient unable to move arm on his own) as well passive movements (examiner unable to move patient’s arm at the shoulder movements of the arm performed by the examiner). In a severe case, all movements of the shoulder are affected (global restriction of shoulder motion).The disease This condition tends to progresses in stages.
1. Stage one (freezing or painful phase): The “freezing” or painful stage,which may last from 6 weeks to 9 months, and in which the patient has a slow onset of pain. As the pain worsens, the shoulder loses its movement.This stage is characterized by slow onset of pain. As the pain worsens, the shoulder loses its movement. This stage may last from 6 weeks to 9 months.
2. Stage two (frozen or adhesive phase): The “frozen” or adhesive This stage is marked by a slow improvement in pain, but the stiffness remains. This stage generally lasts from 4 months to 9 months.
3. Stage three (thawing or recovery phase): The “thawing” or recovery stage,This is the stage during which shoulder motion movement slowly returns towards normal. This stage generally lasts from 5 months to 26 months.
Are there any specific tests to diagnose Frozen shoulder?
There are no specific laboratory tests or investigations which will clinch the diagnosis of frozen shoulder. It is a diagnosis made on the basis of history of patient’s symptoms of pain and stiffness, and findings of global restriction of active as well as passive movements of shoulder on physical examination. Typically, X-rays and MRI scans of shoulder are normal in a case of primary frozen shoulder. These tests may be ordered in order to rule out other causes of shoulder pain and stiffness (like rotator cuff tears).
What is the treatment for Frozen shoulder?
It is generally believed that frozen shoulder is a self limiting condition i.e. it will resolve itself over a period of time (a condition which will resolve on its own). However some patients may need some supportive treatment for alleviation of pain and stiffness during the active phases of the disease. In patients in whom it fails to resolve on its own, or in those with severe disability because of the pain and stiffness, a more aggressive line of treatment may be necessary. The treatment modalities are:
1. Medication: This includes use of anti-inflammatory drugs for pain relief. It should be noted that these medicines do not alter the course of the disease but only suppress the pain. They should be used judiciously under advice of your doctor to avoid adverse side-effects.
2. Physiotherapy: This includes:-
a. Heat treatment modalities like SWD and IFT for pain relief
b. Stretching exercises for regaining movement in the stiff shoulder. These should be initiated after pain is controlled by medication, heat treatment or a cortisone injection.
c. Strengthening exercises for regaining the muscle strength. These are initiated after significant pain relief is achieved with one of the above modalities.
3. Cortisone injection: This is a steroid injection. It may give dramatic pain relief when given in stages 1 & 2 of the disease. This may be given in the gleno-humeral joint (shoulder joint) or in the subacromial space or both. Usually one injection suffices. At times another injection may be required after an interval of 2-3 weeks.
4. Manipulation under anaesthesia (MUA): This involves using gentle and controlled force to break the adhesions to gain some movement in the shoulder. It is performed with the patient under general anaesthesia. It is usually undertaken in the second stage of the disease when the pain and inflammation in the shoulder have settled down. Manipulation has to done with due caution as there is a risk of causing rotator cuff tears and fracture of the humerus during manipulation.
5. Arthroscopic surgery: This involves doing a synovectomy (removal of inflamed inner lining of the shoulder) and capsular release using an arthroscopic shaver. Arthroscopic surgery has the advantage of being minimally invasive in nature, and is not associated with the risk of causing a fracture of the humerus or a rotator cuff tear. Additionally, it allows a complete visualization of the shoulder joint and subacromial space, and to deal with any other associated pathology like a rotator cuff tear.
Case illustration:
This illustration is a case of a 45 year old non-diabetic lady with left sided frozen shoulder. She had been treated with pain medication, physiotherapy and cortisone injection for nearly 9 months without much success. She was treated with Arthroscopic debridement and capsular release with good pain relief and full shoulder function.

